- Scan to follow

- WeChat Service


- WeChat Subscription
Team from School of Public Health of HUST: All the Interventions Performed after the Lockdown of Wuhan Effectively Reduced the Total Number of Infections by 96%
Source:Original Author:admin Time:2020-09-16 View:81The guests of the Nth Dimension of Parallel Future today are Professor Wang Chaolong and Professor Wu Tangchun from School of Public Health of HUST and their team. During the outbreak of COVID-19, the team published multiple relevant academic papers, proposing that the new coronavirus strain spreads in a highly infectious and elusive way. The team drew public attention due to its thesis on “the asymptomatic case” published in Nature, and demonstrated with a model that all the interventions performed after the lockdown of Wuhan effectively controlled the large-scale outbreak of COVID-19.
Let’s review the whole development process of the COVID-19 pandemic through the in-depth analysis by Professor Wang Chaolong and Professor Wu Tangchun.

This article has a total of 4,889 words, and the recommended reading time is 10 minutes.
Wuhan took only 76 days to turn from “pause” to “restart”. Let’s review the key time nodes of the anti-pandemic measures.
Wuhan welcomed a new start after the 76-day lockdown due to COVID-19. The battle against COVID-19 was tough. What are the key time nodes of the anti-pandemic measures implemented by Wuhan, as the first major city severely affected by the pandemic, without special medicines or vaccines? How did these measures influence the pandemic trend? Could they offer some experience for the global fight against COVID-19? On April 10, the expert teams from School of Public Health, Tongji Medical College, Huazhong University of Science and Technology, Fudan University and Harvard University systematically sorted out and summarized the statistics on the pandemic in Wuhan. The research thesis published in The Journal of the American Medical Association (JAMA) answered these questions.
The research incorporated the 32,583 COVID-19 cases with confirmed diagnosis by laboratories from December 8, 2019 to March 8, 2020, and divided the 3-month period into 5 phases according to the key time nodes of the public health interventions (Figure 1):
Phase 1 (before January 10): Early stage of the outbreak of COVID-19; patients and the close contacts were quarantined, but no targeted large-scale interventions were performed;
Phase 2 (January 10 to 22): People flow increased dramatically due to the Spring Festival travel rush, and the virus spread in a relatively fast speed. Before the announcement of human-to-human transmission and infection of medical workers on January 20, few substantial large-scale interventions were performed. On January 20, COVID-19 was incorporated in the system for the direct reporting of infectious diseases. As a Category B infectious disease, it was, however, managed as a Category A infectious disease, which aimed to upgrade the emergency response level of the public health emergencies;
Phase 3 (January 23 to February 1): Departure channels of Wuhan were closed; city-wide traffic control was implemented; public transportation was totally suspended; social activities in clusters were cancelled; and masks were required to be worn in public places. During this period, the construction of Leishenshan Hospital and Huoshenshan Hospital began in succession. Major hospitals quickly figured out ways to renovate their wards to provide more beds for COVID-19 cases and suspected cases; the hospital laboratories and some commercial laboratories were approved to rapidly offer testing services for significant improvement in testing capacity, and medical workers from all over China raced against the clock to assist Wuhan successively.
Phase 4 (February 2 to 16): Medical conditions and resources had been significantly improved. Leishenshan Hospital and Huoshenshan Hospital were put into use successively; the construction of multiple “makeshift hospitals” was completed in a short period with patients quickly hospitalized, and more than 30,000 medical workers rushed to Wuhan to help. Patients were quarantined and treated in designated facilities by classification on the basis of their clinical situations to enhance the nucleic acid testing capacity.
Phase 5 (February 17 to March 8): Massive dragnet screening of potential virus carriers and strong prevention and control measures as before were implemented. The daily nucleic acid testing capacity of Wuhan reached 20,000 around February 20, and the number of discharged cases were increasing. On March 1, the first makeshift hospital was closed; on March 10, all makeshift hospitals accomplished their historical mission.
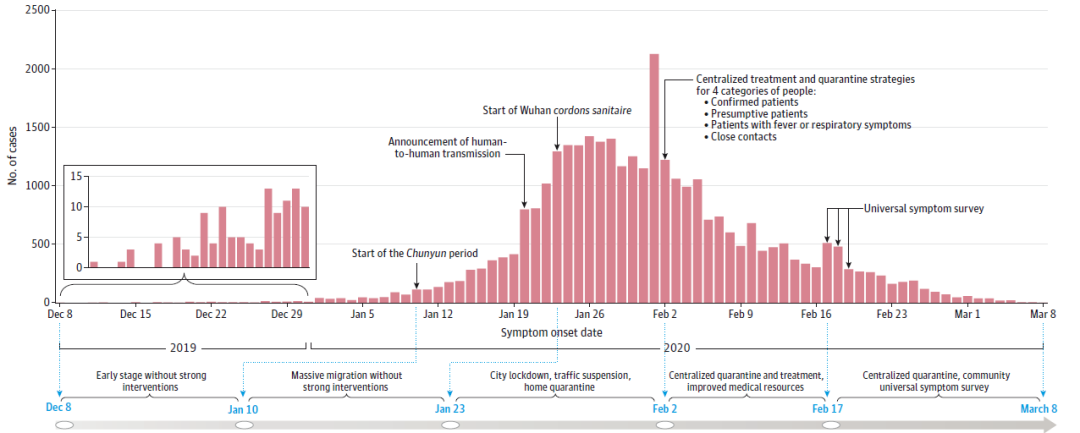
Figure 1: Daily confirmed cases in Wuhan and the time nodes of the 5 anti-pandemic phases during the 3-month period. Source: Pan A et al, JAMA, 2020
Risk of severe or critical symptoms: Increases as people get older, and the proportion of males suffering from this was higher than that of females.
The analytical results showed that with the continuous upgrading and improvement of prevention and control measures, the number of COVID-19 cases and the incidence of the disease continued to decline after reaching the peak in Phase 3. The effective regeneration number (Rt) of COVID-19 reached its peak on January 24 by 3.82, and then dropped below 1.0 on February 6, indicating that the COVID-19 pandemic had been effectively controlled. Then it has been further decreased to below 0.3 since March (Figure 2). Rt is a key indicator reflecting the rate of virus infection, representing the average number of secondary cases caused by a single infectious case during a certain period. When Rt>1, the disease may continue to spread among people, and when Rt<1, the infectious disease will be controlled, and may not continue to spread.
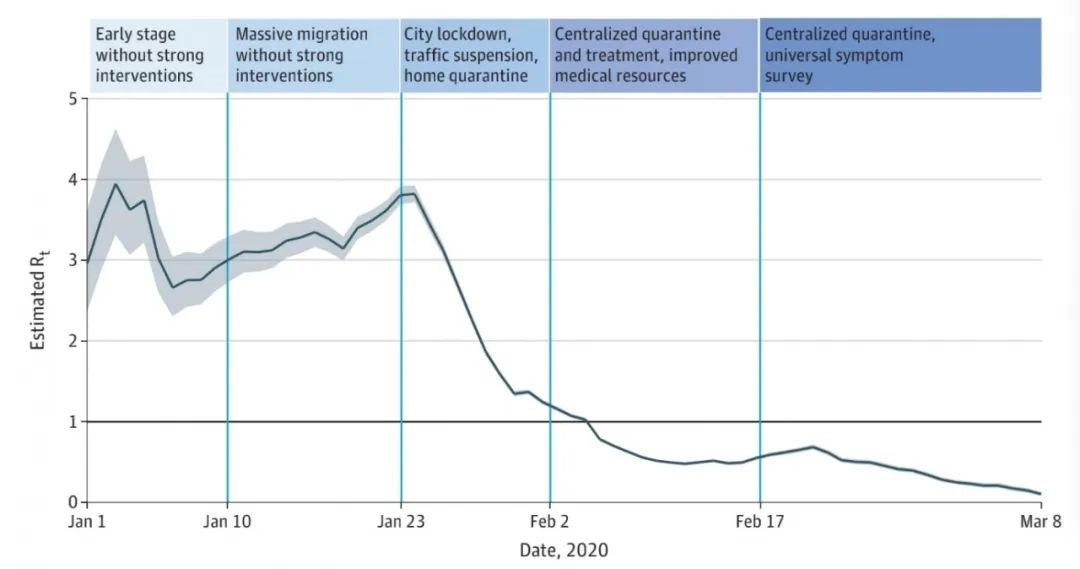 Figure 2: Rt values in the 5 phases. With the gradual upgrading of anti-pandemic measures, the Rt value dropped below 1 in Phase 4 and Phase 5, and the pandemic trend was under control. Source: Pan A et al, JAMA, 2020
Figure 2: Rt values in the 5 phases. With the gradual upgrading of anti-pandemic measures, the Rt value dropped below 1 in Phase 4 and Phase 5, and the pandemic trend was under control. Source: Pan A et al, JAMA, 2020
In addition, the proportion of severe and critical cases continuously declined with time from 53.1% in Phase 1 to 10.3% in Phase 5. Aging was the main risk factor for severe cases: The risk increases as people get older, and males were more likely to have severe symptoms than females (Figure 3).
It was crucial to protect the medical workers in the prevention and control system.
The research also fully demonstrated the importance of protecting the medical workers, which was a crucial link in the pandemic prevention and control system. The research showed that the incidence of COVID-19 in local medical workers was higher than that in the general public, especially in Phase 2 and Phase 3, when the incidence in local medical workers was over 3 times of that in the general public. This also demonstrated that as high-risk staff, medical workers may be at high risk of infection in the early stage of the outbreak of an emerging infectious disease when protection is insufficient. In Phase 4 and Phase 5, with the significant improvement in medical resources and more than 30,000 medical workers raced against the clock to assist Wuhan from all over China, the incidence in local medical workers in Wuhan quickly decreased, which had been close to that of the general public in Phase 5 (Figure 3).
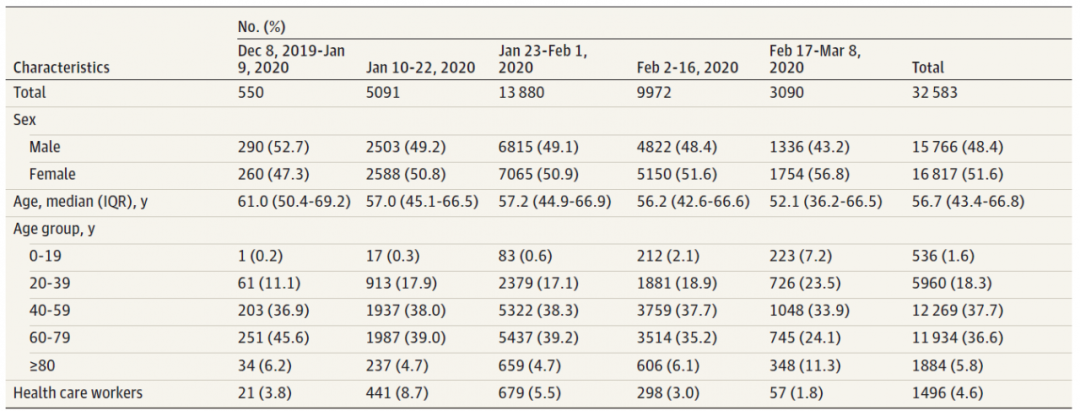 Figure 3: Age and gender of the confirmed patients with the percentage indicated, and the number and proportion of confirmed medical workers in the 5 phases. Source: Pan A et al, JAMA, 2020
Figure 3: Age and gender of the confirmed patients with the percentage indicated, and the number and proportion of confirmed medical workers in the 5 phases. Source: Pan A et al, JAMA, 2020
Centralized quarantine was an important approach to protect the susceptible population.
In terms of the susceptible population, the research found out that children and adolescents under the age of 20 were at a lower risk of infection than other age groups. However, while the incidence of other age groups decreased over time, the incidence of children and teenagers was increasing, especially for babies younger than 1 year old (Figure 3). This also reflected that the risk of infection within the family was increasing with the implementation of control measures, especially the home quarantine requirements. However, children and adolescents had a lower proportion of severe symptoms. Comparatively speaking, the elderly had a relatively high proportion of severe symptoms and thus required special attention.
Constructing “makeshift hospitals” for centralized quarantine was right an important approach to protect the susceptible population. In Phase 4, Wuhan started to convert large utilities such as exhibition halls and gymnasiums into “makeshift hospitals” on February 3, which offered over 13,000 beds for the centralized quarantine and treatment of patients in different phases. The specific quarantine scheme was to send patients with mild symptoms to makeshift hospitals, and patients with severe symptoms to Leishenshan Hospital, Huoshenshan Hospital and designated hospitals. Suspected patients, patients with fever, and close contacts were kept in quarantine separately in hotels, dormitories, and other places. With the implementation of these measures, the risk of cross infection was quickly reduced.
Meanwhile, measures including closed communities, the stay-at-home practice, and centralized distribution of daily necessities were implemented for communities and ordinary citizens to further reduce the risk of community infection.
The team indicated that due to the elusiveness of COVID-19, it may be difficult for us to find all the infected people. The lockdown of Wuhan effectively cut off the transmission channels and reduced the effective infectivity of the virus, thereby bringing the pandemic under control.
The mathematical model for assessment demonstrated again that all the interventions performed after the lockdown of Wuhan effectively reduced the total number of infections by 96.0%
On July 16, 2020, Professor Wang Chaolong and Professor Wu Tangchun at School of Public Health, Tongji Medical College, Huazhong University of Science and Technology published Reconstruction of the Full Transmission Dynamics of COVID-19 in Wuhan in Nature in partnership with Professor Lin Xihong at the Harvard T.H. Chan School of Public Health (with Doctor Hao Xingjie, Associate Professor Cheng Shanshan and Doctor Wu Degang as the co–first authors as well). The research conducted based on the thesis published by the same team in JAMA in April which summarized the relationship between the public health interventions in Wuhan and the pandemic trend further assessed the effectiveness of the prevention and control measures with a mathematical model, and revealed the transmission characteristics of COVID-19, which were helpful for countries all around the world to develop preventive policies and schemes more effectively, and offered valuable guidance for China to finally win the fight against the pandemic and deal with the potential emerging infectious diseases in the future.

Based on the classic SEIR model, in view of the known characteristics of COVID-19, including already being infectious before the symptoms are shown, the imperceptibility of a large number of infections due to the mildness of the symptoms, and the lower infectivity of patients with mild symptoms, and taking into account the changes in population flow and intervention intensity in different stages, a dynamic analysis model named SAPHIRE was proposed to perform fitting and parameter estimation for the pandemic trend curve of Wuhan as of March 8. Through the model comparison, the research estimated that all the intervention measures implemented after the lockdown of Wuhan on January 23 effectively reduced the total number of infections as of March 8 by 96.0%, and the interventions performed since February 2 such as the centralized quarantine of “the four groups of people” reduced the number of infections by 69.6% (Figure 4). The results showed that the joint prevention and control was highly effective, and successfully protected the lives and health of the public. According to the two professors from the team, the model estimated that the number of infections as of March 8 would have been 25 times of the actual number if Wuhan had not been locked down on January 23, and no interventions had been performed, allowing the virus to spread. However, their model was unable to separately assess the effectiveness of the lockdown.

Figure 4: Trend fitting and prediction of the daily confirmed cases under different conditions: (a) fitting of the actual situation; (b) trend prediction on the assumption that the massive screening started from February 17 was not conducted; (c) trend prediction on the assumption that measures including the centralized quarantine put into practice on February 2 were not implemented; (d) trend prediction on the assumption that no interventions were performed.
Integrated measures including the mask-wearing rules for all people and social distancing effectively contained the spread of COVID-19.
The model research revealed the two major features of COVID-19: high infectivity and high elusiveness. In early phases when no interventions had been performed, the regeneration coefficient (R) of COVID-19 was as high as 3.54, indicating that its infectivity is much higher than known coronaviruses such as SARS and MERS. After intervention measures were implemented on January 23, the R value dropped significantly to 1.18, and the increase of the number of daily confirmed cases slowed down. After centralized quarantine was put into practice on February 2, the R value further dropped to 0.51, and the number of daily confirmed cases started to decrease day by day. After the massive community screening from February 17 to 19 that further reduced the sources of infection in communities, the R value dropped to 0.28, significantly shortening the time required to achieve the goal of “zero infection”. The model estimated that about 87% (with a lower limit of 53%) of the patients with COVID-19 had not been confirmed as of March 8 due to asymptomatic or imperceptible symptoms, and the infection rate of the corresponding groups was about 2.5%. Although the infectivity of unconfirmed cases set in the model in accordance with the references was only half of that of the confirmed cases, it may be an important driver of the early development of the pandemic due to their high proportion. In later phases, although these infections were not confirmed and quarantined, their infectivity was significantly limited as comprehensive measures including the mask-wearing rules for all people and social distancing effectively cut off the transmission channels, and the number of these infections gradually decreased through self-cure (Figure 5). Multiple recent serological studies published by European and American countries also found out that the proportion of Wuhan natives tested positive for COVID-19 antibodies was much higher than the proportion of confirmed COVID-19 patients, which was basically consistent with the results of this research, revealing the high elusiveness of COVID-19. Furthermore, the results of the serological study published by the team of Academician Hou Fanfan from Southern Medical University in Nature Medicine on June 5 showed that about 3.2 to 3.8% of the medical workers in Wuhan, their relatives, and the employees of the hotels they stayed in were tested positive for COVID-19 antibodies, while the actual infection rate in the general population needed to be confirmed through more extensive serological studies.
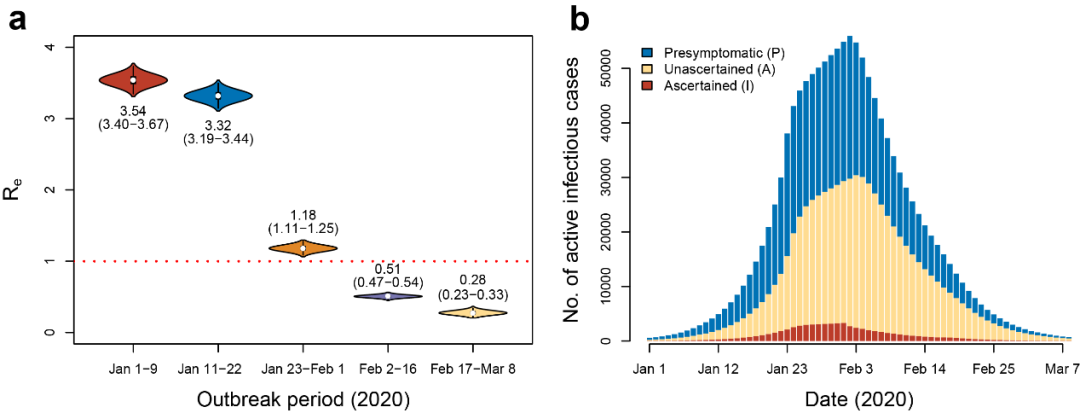 Figure 5: Transmission characteristics of COVID-19: (a) Effective regeneration coefficient in different phases; (b) Total number of the active daily sources of infection and the composition.
Figure 5: Transmission characteristics of COVID-19: (a) Effective regeneration coefficient in different phases; (b) Total number of the active daily sources of infection and the composition.
COVID-19 is quite cunning, and continued monitoring is required to prevent its resurgence.
The high infectivity and high elusiveness of COVID-19 have greatly increased the difficulty of pandemic prevention and control, and explained the reason why the virus can spread rapidly all around the world. The research made further prediction with the model to assess the probability of the resurgence of the pandemic on the assumption that prevention and control measures are lifted under different conditions (Figure 6). The probability of a second wave of the pandemic will be 32% if all prevention and control measures are lifted under the condition that 87% of the infections are not detected and no confirmed cases are seen for 14 consecutive days. If only 53% of the infections are not detected, the probability of the resurgence of the pandemic will drop to 6% correspondingly. The probability of the second outbreak of the pandemic will increase significantly if the prevention and control measures are lifted too early. The results indicate that in the face of the cunning and elusive COVID-19, we should keep monitoring the pandemic while resuming work and production to restore economic order, and quickly adjust the prevention and control measures based on the pandemic trend to prevent a secondary outbreak. These research findings shed bright light on global pandemic prevention and control and the formulation of corresponding public health policies in various counties.
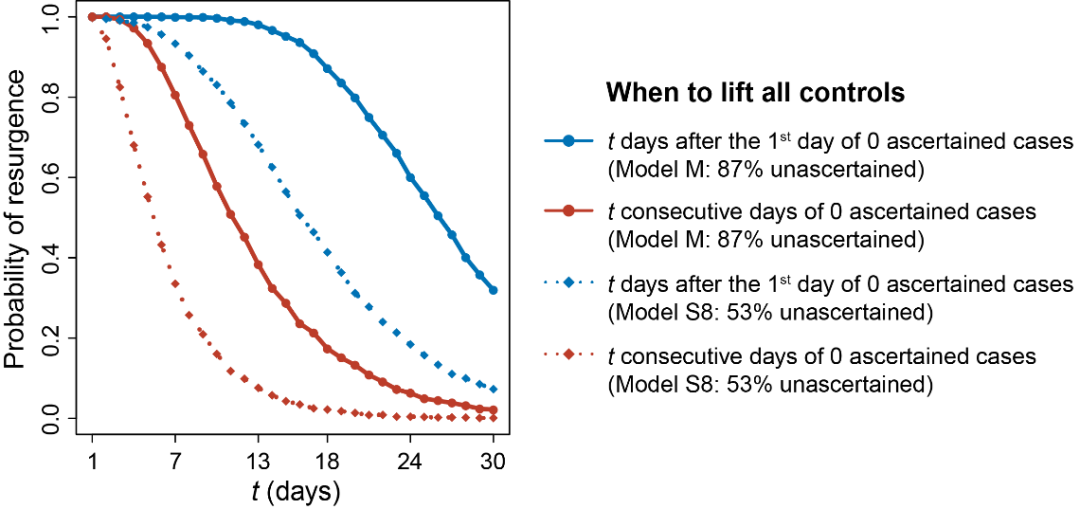
Figure 6 Risk of the resurgence of the pandemic on the assumption that all prevention and control measure are lifted under different conditions.
Most of the asymptomatic patients may cure themselves with their own immunity systems.
Nature published an article titled Covert Coronavirus Infections Could Be Seeding New Outbreaks as early as in March, indicating that 30% to 60% of the COVID-9 patients had no or mild symptoms, but their infectivity was not low, and these covert infections may cause a new round of outbreak. The thesis attracted public attention instantly.
As a member of the thesis team, Professor Wu Tangchun indicated that according to their most conservative estimation, at least 59% of the infected people had not been tested, and may infect others. This may explain why the virus spread so fast.
In the interview, he and Professor Wang Chaolong further revealed that most of the asymptomatic patients and patients with mild symptoms may kill the virus and cure themselves with their own immune systems.
Asymptomatic infection may not be a good thing?
Through a recent study by Chongqing Medical University, Chongqing Wanzhou Center for Disease Control and Prevention, Chongqing Wanzhou People’s Hospital and Chongqing Center for Disease Control and Prevention, the researchers found out that people who are infected with SARS-CoV-2 (the novel coronavirus that causes COVID-19) but show no symptoms may have a lower level of immunity to the virus than those with severe symptoms, which sparked a heated discussion that “asymptomatic infection may not be a good thing”. The two professors indicated that the so-called lower level of immunity only indicates that the antibody level detected in the human body is relatively low. For the asymptomatic patients and patients with mild symptoms, their organs may not be severely invaded by the virus. For this reason, no strong immune responses will be induced, so the lower antibody level is understandable. It is a good thing as long as the virus can be killed by the human body without causing major health damage to the human body.
Virus mutation is the result of a random process of natural evolution.
Whether COVID-19 will mutate is also a hot topic in the society. This June, mutated COVID-19 virus appeared in Tokyo and diffused across the city, and the virus found in Beijing before had also mutated. In only a few months since the outbreak of COVID-19, the virus has mutated many times, which means that we will be in a passive defense state for a long time if we cannot predict the direction of virus mutation. In this regard, the two professors expressed their opinions in the interview as follows: Virus mutation is a normal biological phenomenon. Most of the mutations will not bring about changes in biological properties, but only a few mutations may cause functional changes. The mutation studies by biologists focus mainly on a small number of variations that may cause functional changes. Virus mutation is the result of a random process of natural evolution, so we have no way to know the direction of mutation in advance.
- 12023 PIF | Brazil has been invited as the Country of HonorPujiang Innovation Forum
- 2Postponement of 2022 Pujiang Innovation Forum (15th)Pujiang Innovation Forum
- 3Collection of Global Practical Cases of Low-carbon InnovationPujiang Innovation Forum
- 4Special Sub-Forum | Focus on innovation cooperation, innovation trends, innovation vitalityPujiang Innovation Forum
- 5Stunning Highlight | Shaanxi Will Step onto the Stage of 2020 Pujiang Innovation Forum as the Province of HonorPujiang Innovation Forum
- 6Team from School of Public Health of HUST: All the Interventions Performed after the Lockdown of Wuhan Effectively Reduced the Total Number of Infections by 96%Pujiang Innovation Forum
- 7Experts address global warming during science eventPujiang Innovation Forum
- 8Special Conversation with Lu Xi from Shanghai Academy of Spaceflight Technology (Part 2): "Is Mars Colonization Promising?"Pujiang Innovation Forum
- 9Special Conversation with Lu Xi from Shanghai Academy of Spaceflight Technology: “Hello, Mars”Pujiang Innovation Forum
- 10Seeking Insights into the Future Trends and the Road to Innovation at Pujiang Innovation ForumPujiang Innovation Forum

